We’ve all been there before – looking in the mirror to find an angry, red, inflamed pimple. It looks nasty. It feels painful, and the worst part? Popping it will only make it worse.
Have you ever wondered what causes these pimples to form in the first place?
Your dermatologist might tell you that you’re using the wrong cleansers or products, but the real cause of these pimples are nutritional deficiencies that lead to chronic inflammation.
Chronic inflammation one of the root causes of acne and affects millions of Americans every year. It can be triggered by extremely common ingredients found in everyday foods like low-fat yogurt, protein bars, and salad dressings. It’s no surprise that both rates of chronic inflammation and acne are at all-time highs (R).
The good news? Stopping chronic inflammation is as easy as making a few simple changes to your diet and lifestyle. Not only will your skin clear up, but you’ll probably feel better both mentally and physically too.
I’ll guide you through how to stop chronic inflammation, but first, we need to understand what chronic inflammation is.
What is inflammation?
Inflammation is the body’s natural response to foreign invaders, like toxins, bacteria, viruses, and physical damage. In moderation, inflammation is a good thing. When you get a cut or bruise, inflammation is your body’s way of making sure it doesn’t get infected. You wouldn’t survive if it wasn’t for inflammation.
There are two main types of inflammation:
- The good, healthy inflammation is called acute inflammation.
- The acne-causing, unhealthy inflammation is called chronic inflammation.
Chronic just means persistent, or recurring. So “chronic” inflammation means inflammation that won’t go away.

With chronic inflammation, your immune system (which responds to threats like viruses, bacteria, and other foreign invaders) is overly active. It treats everything like a major threat, even if it really isn’t dangerous. Stress, naturally-occurring infections, and even certain foods become sources of inflammation. These are routine bodily functions, but because of an overactive immune system, your body responds to them like serious threats.
One of these “harmless biological functions” your body overreacts to is acne.
How does chronic inflammation cause acne?
An acne infection isn’t all that dangerous or threatening to the body. It doesn’t take a large inflammatory response to make sure no damage is done – but when you suffer from chronic inflammation, your body thinks any infection is a huge threat.
Even small acne infections caused by a blocked pore puts your immune system on high alert. Tons of pro-inflammatory cells called cytokines are sent to the pore to clean up the mess. In order to stop this harmless acne infection, your body responds as if it were a serious cut or injury – by producing a red, protruding, inflamed comedo.
Sound familiar? That’s because the process of chronic inflammation is largely behind pimples and whiteheads.
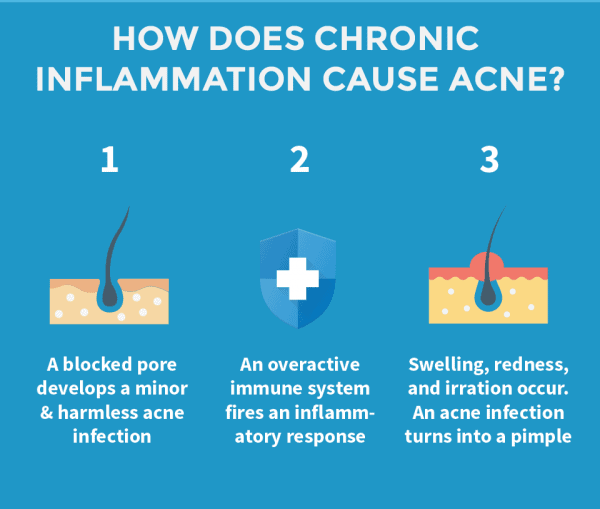
This is a deeply-rooted process that starts beneath the surface of the skin. Using harsh chemical cleansers or a new face mask won’t stop chronic inflammation. That’s why it’s crucial to tackle acne at the source: by fixing the dietary imbalances that lead to chronic inflammation.
What causes chronic inflammation?
Just like the other root causes of acne, chronic inflammation is largely a side-effect of our modern diet and lifestyle. The main culprit: our increased consumption of unhealthy fats and grains.
Cause #1: Eating too many pro-inflammatory fats
Unfortunately, you’ve been lied to. For years the USDA told us that in order to be healthy, we need to avoid fats and instead eat plenty of whole grains, rice, and pasta. The end result is that we’ve replaced healthy saturated fats (like coconut oil, extra-virgin olive oil, and ghee butter) with unhealthy, acne-causing industrial fats (like vegetable oils and margarine).
Why?
Because they look a lot better on a nutrition label. If you still believe that “fat is evil”, then unhealthy, processed, low-fat vegetable oils, like canola, corn, or sunflower oil, seem like they’re a lot better for you than healthy, saturated fats like coconut or olive oil. In reality, the exact opposite is true.
Saturated fat isn’t evil, and by replacing them with vegetable oils we’ve developed widespread chronic inflammation.
For more info on fats as a whole, I recommend reading this article.

But what’s so unhealthy about these oils? Why should you opt for real fats whenever possible? It all comes down to the all-important omega ratio. Balancing your consumption of omega-6 fats (inflammatory, acne-causing) with omega-3 fats (anti-inflammatory, skin-clearing) is one of the keys to clear skin.
Omega-3s vs. Omega-6s
In the world of fats, there are 3 basic categories: saturated fats, monounsaturated fats, and polyunsaturated fats. Just about every food that contains fat has all three types in different amounts. For now, we’re worried about polyunsaturated fats, or PUFA’s for short.
Within polyunsaturated fats, there are two important sub-categories that affect your body’s inflammatory response, and they’re extremely important to know for acne:
- Omega-3 Fats – Anti-inflammatory. More Omega-3s = Less Inflammation = Less Acne
- Omega-6 Fats – Pro-inflammatory. More Omega-6s = More Inflammation = More acne
Your body needs both fats to thrive. Omega-6 isn’t completely evil – it’s necessary for brain development, hair growth, and a well-functioning immune system. Too much omega-6 is where the problems start.

Unfortunately, our modern diets consist of way too much omega-6 and not nearly enough omega-3. The end result is chronic inflammation.
What’s Your Omega Ratio?
Before we started consuming vegetable oils and trans fats, it’s estimated that our omega ratio, or the amount of omega 6 fats we consumed versus the amount of omega 3 fats, was somewhere around 1:1, meaning we ate equal amounts of omega-3s and omega-6s. Some estimates say it was closer to 2:1, meaning we ate 2x as many omega-6s.
For clear skin, an omega ratio of somewhere between 2:1 and 4:1 is ideal, meaning you want to consume no more than 2-4x as much omega-6 as omega-3.

Where would you guess your omega ratio is at?
If you’re like most Americans, it’s probably a shocking 10:1 or more (R).
Diets high in omega-6 fatty acids compared to omega-3 fatty acids affect just about every aspect of our health:
- Increased risk of cardiovascular disease (R)
- Increased risk of cancer (R)
- Increased risk of autoimmune disorders (R)
Unless you already eat extremely clean and have eliminated all vegetable oils from your diet, you’re probably pumping your body full of inflammation-causing fats without even knowing it.
The reason for this is simple – industrial fats are everywhere, and they’re packed with omega-6:
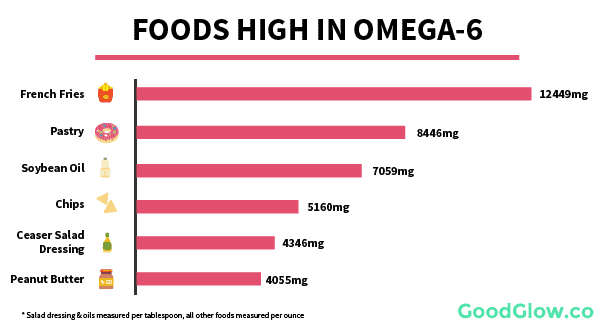
If you take one thing away from this article, let it be this: avoid foods high in omega-6.
Cause #2: An unhealthy gut
High consumption of omega-6 isn’t the only culprit for chronic inflammation. A damaged or unhealthy digestive system can also be a huge factor, especially if you have leaky gut syndrome.
Leaky gut syndrome is when the lining of your intestine becomes damaged and allows certain chemicals and nutrients to “leak” into your bloodstream. Once these chemicals are in your bloodstream, your body triggers a standard inflammatory response to fight the “threat”. It’s easy to see why this is a problem – if an inflammatory response is being triggered every time you eat, it’s nearly impossible to avoid chronic inflammation.
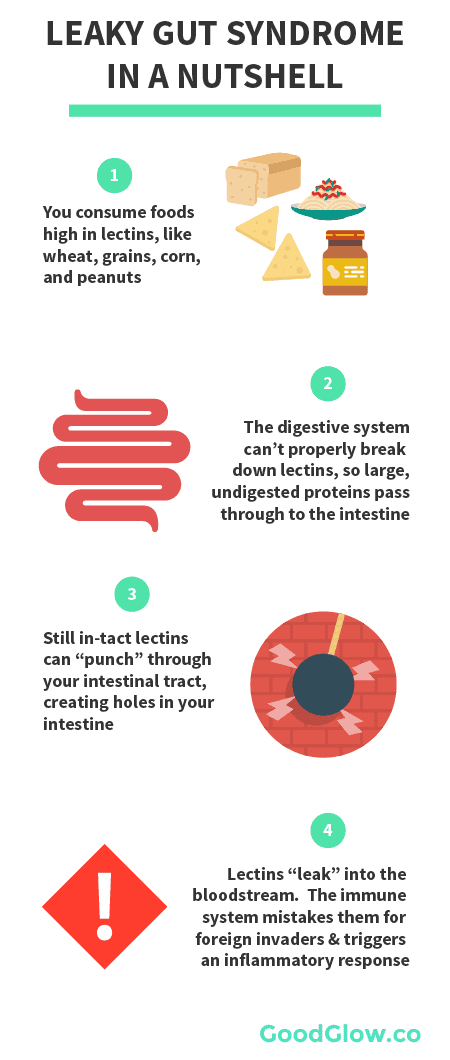
But what causes leaky gut syndrome in the first place?
Usually, it’s built up over years due to the repeated consumption of potent antinutrients called lectins.
Most of the foods we eat have lectins in them, and in moderate doses, they pose no real threat. Plants use lectins to protect themselves from being eaten in the wild – it’s their best attempt to make themselves indigestible in order to fight off any predators. If a berry has potent enough lectins to make a squirrel trying to eat it sick, then the berry survives and reproduces (and the squirrel’s buddies take note: don’t f*ck with those berries).
Just about every plant or seed has lectins in it. Some of them we can handle really well, like the lectins found in most fruits and vegetables. Some of them we really can’t handle, and they enter our intestine totally undigested. These undigested lectins can actually permeate, or penetrate, our intestinal wall and enter our bloodstream. In other words, they “punch holes” in our gut.
Yikes, that’s not good.
When this intestinal wall continues to become weaker and weaker, more and more foods can pass through and trigger an inflammatory response. That’s why people with leaky gut syndrome may become intolerant to foods they’d otherwise be fine with – eggs, meats, certain vegetables, etc.
Avoiding lectins is a must for chronic inflammation. Potent lectins include wheat, peanuts, legumes, and other grains (quinoa, oats, barley, etc.).
Cause #3: Lifestyle factors like stress and sleep
Stress, sleep, and exercise touch just about every possible aspect of your health, including inflammation:
- Stress is like inflammation – it’s necessary for survival and (in small doses) can be a good thing! For thousands of years, stress has triggered an inflammatory response that helps us fight off physical threats. That’s great! But what about when that “threat” is traffic, social anxiety, or a work deadline? That’s when you run into issues. Studies show that these minor psychological threats trigger pro-inflammatory responses that lead to chronic inflammation (R). Read my article here about how meditation can help decrease chronic stress.
- Sleep deprivation is a nightmare for your health and acne, so it’s no surprise that inflammation has something to do with it. Inadequate sleep can trigger inflammation and also decrease gut health, which can lead to leaky gut syndrome and trigger even more inflammation (R).
- Exercise causes acute inflammation, the good kind of inflammation, and also decreases chronic inflammation. Just 20 minutes a day of exercise has been shown to decrease inflammation and insulin resistance (R).
Now that you know what causes chronic inflammation, it’s time to dig into the things you can do to stop it.
How can I fight chronic inflammation?
Combating chronic inflammation isn’t too difficult – with a few dietary tweaks you can easily turn the tides in your favor.

Strategy #1: Avoid vegetable oils and industrial fats
Getting rid of all unhealthy fats loaded with omega-6 should be your first (and easiest) step towards beating chronic inflammation.
Here’s the complete list of vegetable oils to avoid:
- Canola oil
- Soybean Oil
- Wheat germ oil
- Corn oil
- Sesame oil
- Sunflower oil
- Peanut oil
- Cottonseed oil
- Grapeseed oil
- Margarine
- Shortening
It’s not just cooking oils you need to be careful of – you can find these oils in just about every processed food known to man. Always check the ingredients list. A decent rule of thumb is that if it’s cheap and comes wrapped in plastic, it probably has vegetable oils in it. Here’s a common list of processed foods that often contain industrial fats:

If you cook with these oils, switch to omega-balanced alternatives like extra-virgin olive oil, extra-virgin coconut oil, avocado oil, or grass-fed ghee butter. They might cost a bit more, but the taste and nutritional benefits are worth it.
If you’re looking for solid salad dressing replacements, the “Primal Kitchen” brand actually has pretty tasty dressings that use healthy fats, including avocado oil, cage-free eggs, and organic apple cider vinegar. I’m a big fan of their Green Goddess.
It’s important to point out that there are some natural vegetable seed oils that can help reduce inflammation and naturally clear your skin. A few examples are tea tree oil, black seed oil, and pumpkin seed oil. While none of these are “magic bullets” for eliminating inflammation or acne they can be beneficial in their raw, naturally occurring form. Pumpkin seed oil in particular is beneficial for cleaning sebum out of large pores.
Strategy #2: Eat more healthy fats
Limiting omega-6s is half the equation, but increasing omega-3 consumption through your diet or with supplements is also crucial for clear skin.
The best way to do this? Eat more fish. Fish like sardines and salmon are packed with omega-3s and have very little omega-6s.
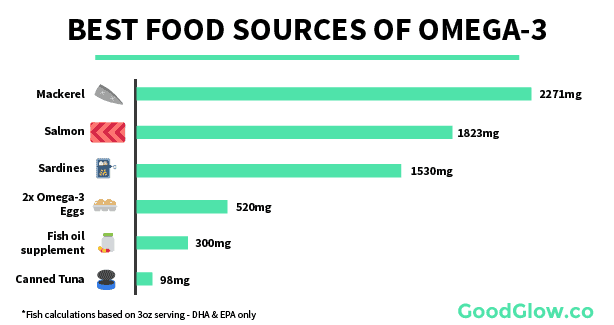
The more omega-3 you can get through your diet, the less likely it’ll be that omega-6 fatty acids will trigger chronic inflammation.
It’s important to note that there are a few different kinds of omega-3 fatty acids, and not all of them are created equal. DHA & EPA are forms of omega-3 that your body can easily use for regulating inflammation, improving the nervous system, and enhancing sleep, muscle growth, and insulin sensitivity. These are the two omega-3s you really want to focus on. The only foods really high in DHA & EPA is fish (and fish oil).
ALA omega-3, on the other hand, is pretty much useless – ALA is found primarily in plants and isn’t easily absorbed or used by the body. While you might consume 200mg of ALA omega-3, in reality only a tiny fraction of that will be converted to usable omega-3 fatty acids. That’s why it’s crucial that if you’re not eating wild-caught seafood, you either add it to your diet or start supplementing.
What about nuts?
No conversation about healthy fats is complete without bringing up nuts. Most nuts are very high in omega-6s, however, there are some safe choices.
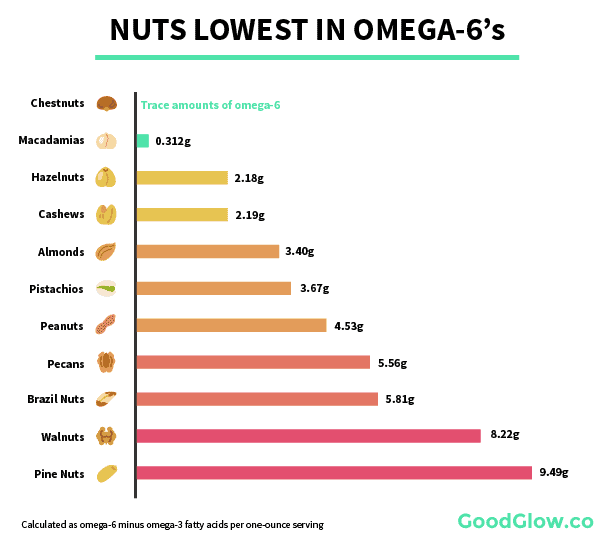
So does this mean you should totally avoid nuts? No, not at all, some nuts are a huge asset for fighting acne, you just need to watch your portion size. Almonds, for instance, are one of the single best sources of the skin-clearing nutrient, vitamin E Brazil nuts are loaded with selenium. Look at nuts as a snack, not a meal, and you’ll be fine.
For more on nuts, read my ultimate guide to nuts for acne-prone skin right here.
What about fish oil supplements?
Do you hate the taste of fish or can’t afford wild-caught seafood? You’re in luck – omega-3 supplements can do the trick, but only if you choose the right kind.

There are 3 main drawbacks to taking a fish oil supplement vs. eating fish:
- You won’t get the other health benefits of eating fish: Like vitamin A, protein, vitamin b12, selenium and vitamin D – all crucial nutrients for acne
- Fish oil goes rancid extremely easily and can make acne worse: One study found that over half of all fish oil brands exceeded the standard for oxidized fat – what does this mean in plain English? They were rancid. Oxidized fats will actually cause inflammation.
- You don’t absorb as much omega-3s: Several studies have shown that the consumption of fish is a much more effective way to increase DHA & EPA (the good omega-3s) levels than fish oil supplements
For these reasons, I’d highly recommend food-based sources of omega-3, like wild-caught salmon, sardines, or canned cod liver oil.
If you’re going to take a fish oil supplement, go with krill oil over other alternates. Krill oil is substantially less fragile than your typical fish oil thanks to a special little antioxidant known as astaxanthin. Astaxanthin prevents krill oil from going rancid due to light or heat exposure. It’s a bit more expensive and you might not get quite as many omega-3s per pill, but it’s a heck of a lot better than consuming rancid pills that cause inflammation instead of preventing it.
I personally use Sports Research Antarctic Krill Oil.
Strategy #3: Avoid wheat, corn, and legumes
If you think wheat, corn, and legumes are “healthy”, think again.
“But what about the food pyramid? Aren’t we supposed to have plenty of whole grains? Aren’t they loaded with fiber?’
While it’s true that whole grains can be a significant source of nutrients like fiber, they also contain really harmful antinutrients known as lectins.
These lectins destroy your gut health and digestive system. They contribute to chronic inflammation, increased insulin resistance, and even leaky gut syndrome. As we’ve talked about already, all of these are a no-go for clear skin. The solution is simple – eat less (bad) lectins!

Wheat isn’t the only category of grains you need to avoid – other pseudo-grains, like oats, barley, quinoa, and even legumes, if not properly cooked, contain tons of lectins too. Peanuts are worth mentioning, as they have a particularly dangerous lectin known as peanut agglutinin which has been shown in studies to disrupt the gut lining.
Other Tips For Decreasing Inflammation
Eat more fermented foods – Sauerkraut, kimchi, and kombucha are all loaded with probiotics and live cultures that contribute to a healthy digestive system.
Take a Zinc Supplement – Zinc is an essential nutrient for fighting chronic inflammation. Unfortunately, it’s really difficult to get enough zinc through diet alone. Taking upwards of 50mg a day of a high-quality zinc picolinate supplement can be a great strategy to keep chronic inflammation at bay.
Get more sleep – It sounds simple, but make sure you’re sleeping enough. Somewhere between 8 and 9 hours is adequate for most adults.
Exercise – Working out causes acute (good) inflammation and helps fight chronic (bad) inflammation and insulin resistance (R).
Try meditation or yoga for stress – More stress means more inflammation. Meditation and yoga are both phenomenal ways to decrease stress and help with acne – for more check out my article on meditation, mindfulness, and acne.
Go for a walk after meals – It sounds simple, but just going for a quick 15-20 minute walk after your meal can aid digestion and decrease insulin resistance (R)
Try intermittent fasting – I wrote an in-depth article about intermittent fasting for acne here. Just skipping breakfast could greatly reduce your inflammation levels.
Putting It All Together
Chronic inflammation is everywhere. With how frequently we consume salad dressings, “low-fat” products, and packaged goods, it’s likely that most of us are overflowing our bodies with omega-6 fats. Worst of all, how often do we really eat wild-caught fish rich in omega-3s to help offset all those unhealthy fats?
Think of all the grains we’re consuming on a daily basis too – our digestive systems aren’t getting a break, and the result is chronic inflammation. Pile on the stresses of modern life and a culture that wears sleep deprivation as a badge of honor and you have the perfect breeding ground for chronic inflammation.
Luckily, you have all the tools you need to stop chronic inflammation at the source. Trust me – if you follow these guidelines, the amount of red, angry, inflamed pimples you have will decrease dramatically:
- Cut out all industrial fats – Salad dressings, processed foods, and vegetable oils are loaded with inflammatory omega-6 fats. Cutting them out can make a huge difference in your skin
- Eat more healthy fats – Wild-caught fish like salmon and sardines or krill oil supplements are jam-packed with skin-clearing omega-3 fats. Eating fish twice a week or supplementing daily can re-balance your omega ratio
- Avoid lectins – Wheat, corn, and legumes are a nightmare for your gut health and can lead to leaky gut syndrome. Cutting out pasta, bread, oats, peanuts, corn, beans, white potatoes, and processed foods are a must for keeping lectins under control.
- Drink lots of water – Water is a natural detoxifier and dehydration is one of the leading causes of inflammation in the body.
When in doubt, start small – cut out conventional salad dressings and opt for vinaigrettes or incorporate some wild-caught salmon into your diet once a week. Once you get the ball rolling, it’ll be easier and easier to make the changes that lead to permanently clear skin.

Can I just say thank you so much for this website. I’ve read books, bought creams, ditched dairy and still could not get rid of my acne. I bought some of the supplements you recommended and cut out most of the foods you recommended as well and it’s been about 3 months now and my face is SO much clearer. I just quit coffee and it’s clearing up even more too. I was so embarrassed about acne that I didn’t even want to go out to town with my husband anymore. It was terrible. I am so thankful for the info you have here. I was to the point of really considering accutane but I was afraid of the side effects. I can not thank you enough. Seriously. Thank you so much.